By Susan Usher, Anita Brown-Johnson, Nadine Larente
This case study, prepared by Health Innovation Forum with contributions from Dr. Anita Brown-Johnson, Dr. Nadine Larente and Mr. Michel Clair, examines the transition care expertise developed at the MUHC and at efforts to effect a smooth transition to faster placements in community resources as new laws take effect. —A case study prepared as part of the 2011 program of the MUHC-ISAI
Challenge
Transition care at the MUHC made progress in reducing acute bed blockages. The challenge now is to ensure that problems do not reappear as these patients are moved into community facilities.
Dr. Anita Brown-Johnson has been the physician in charge of transition care patients at the McGill University Health Centre (MUHC) for more than a decade. These are patients who no longer require acute care but cannot be discharged home and are waiting for an available spot in another facility, be it rehabilitation, long-term care or home care. Dr. Brown-Johnson has introduced new models of hospital care for these patients and has studied patient factors that complicate transfers.
Hospital solutions for transition care patients: The MUHC model
Twelve years ago, the MUHC had a long-term care service comprised of 173 beds allocated across the adult sites (Montreal Chest Institute, Royal Victoria Hospital and Montreal General Hospital). Over time, those beds were progressively decreased to 132 and the name of the units was changed from long-term care to “transition care.” Transition care at the MUHC was meant to provide continuing high quality medical, specialized nursing and other allied healthcare services to patients with complex clinical care needs and reduced autonomy while focusing on discharge planning, psychosocial support and patient/family education to expedite the transfer of patients from the MUHC to more appropriate community resources.
Dr. Brown-Johnson describes a number of measures introduced by the MUHC to reduce the time patients spent on transition-care units.
1. Patients were required to indicate a second choice of long-term care (LTC) facility should their first choice have a waiting time of more than three months. This policy initiated the use of community transition (or temporary placement) beds, and was later adopted by the Regional Health Board (Agence de développement de réseaux locaux de Services de santé et des Services sociaux de Montréal or ADRLSSSM), becoming city-wide policy in 2003-2004.
2. A discharge planning policy for transition-care patients was developed and implemented with careful attention to matching patient needs to appropriate resources in the community in order to prevent the need for readmission to the hospital (usually via the ER).
3. The transition-care service adopted strategies to prepare patients for discharge medically, psychosocially and financially.
4. The transition-care team provided telephone consultations to community LTC partners to support the management of patients with complex care needs, with the objective of reducing avoidable readmissions to hospital.
5. The Office of Post Hospital Care and Community Support (OPHCCS) was created in 2008 to standardize internal processes and procedures and implement best strategies to support timely access to community-based care, in collaboration with clinical teams, the Health and Social Service Centres (CSSS) and the Agence. The OPHCCS supports clinical teams by resolving obstacles to timely discharge and helps community LTC and other partners access specialized care for patients with appartenance at the MUHC.*
MUHC staff have also provided in-service training to staff in LTC facilities to help them cope with problems that would previously have seen the patient return to the ER: unblocking foley catheters and caring for feeding tubes, for example.
“The combination of such measures reduced the length of stay on the transition-care unit of the MUHC from an average of seven months in 2002 to between two and three months in 2009,” says Dr. Brown-Johnson. “The readmission rate was about 1% in 2009, and bounce back to the ER within two weeks of discharge was around 3%. These figures are tracked on the transition care unit’s balanced score card.”
The MUHC’s initiatives have been undertaken in the context of a chronic shortage of long-term beds in the community. It has never in the past been possible to transfer all patients who have completed acute care to an appropriate resource within a short period of time. In the past five years, the Ministère de la Santé et des Services sociaux (MSSS) and the ADRLSSSM have stepped up efforts to provide non-hospital alternatives for these patients in order to relieve congestion in hospitals.
Community solutions
Reducing transition-care stays in hospital requires ensuring that appropriate services are available in the community. In 2006, the ADRLSSSM initiated a series of measures to radically change the process for placement. The strategy involves increasing and improving home-care services in the community; diversifying residential-care possibilities to respond to different levels of need; improving long-term care, intermediate care and residential-care resources through an accreditation and inspection process; enhancing the capacity of LTC resources to provide higher levels of care; and progressively closing LTC and transition-care units in hospitals.
Transferring responsibility
The policy
The ADRLSSSM, following directives from the MSSS, redefined eligibility for placement in LTC facilities. Previously, a LTC facility would admit patients requiring anywhere from one-and-a-half hours to seven hours of nursing care per day. Between 2007 and 2009, the lower limit was progressively increased so that a patient must now require at least three hours of nursing care per day to be eligible for admission. People requiring fewer than three hours of care per day are gradually being moved out of the LTC facilities and into newly created intermediate-care facilities.
Medical and allied healthcare resources are being shifted accordingly. The LTC facilities require additional investments to upgrade the level of care and adjust staffing to meet the needs of patients requiring heavier care. The Ministry has been guiding this transformation since the start of 2009. Intermediate-care facilities do not maintain their own medical or nursing staff, but rely on physicians and nurses at the CSSS in their area.
The practice
The closure of LTC units in hospitals began in 2009 with the aim of shifting patients and budgets to the expanded range of community-based resources. The goal was to progressively close a total of 800 to 900 hospital LTC beds in the Montreal area. St Mary’s Hospital Centre was selected as a test hospital for implementation of Program 68, which has since been renamed “Programme d’hébergement pour évaluation” (or “PHPE”), and started discharging patients in January 2009. In the first six months, the reduction in LTC patients was found to enable new patients to move more quickly through the ER to acute-care beds. In 2009-2010, LTC beds were closed at the Jewish General Hospital, followed by Hôpital Maisonneuve Rosemont (January 2010), the Centre hospitalier universitaire de Montréal or CHUM (April 2010), CSSS/Hôpital de Verdun (August 2010), the MUHC’s Lachine Hospital (August 2010), Hôpital Fleury and Hôpital Jean Talon (December 2011). Implementation is expected at the MUHC’s Royal Victoria and Montreal General hospitals this year.
In a presentation delivered to the Commission de la santé et des services sociaux on August 23, 2011, Mr. David Levine, President and CEO of the ADRLSSSM described progress since 2006 in providing Montreal’s older population with appropriate resources.
By 2011, 554 hospital LTC beds in Montreal were closed. At the same time, a new procedure was put in place whereby the responsibility for coordinating the person’s care was assumed by the local CSSS as soon as active care ceased, and the person was to be transferred within 72 hours to an evaluation bed within a LTC facility. The average stay in this facility was 44 days, during which time the level of need was established. The person was then placed in another LTC facility even if the first choice was not available.
The number of people receiving home care in Montreal increased from 43,000 to almost 50,000 between 2006 and 2011, and 600 intensive home care “places” were created. The effort to improve community LTC facilities saw 525 beds closed and 3,471 modernized, with a net decrease in the number of LTC beds over five years. Ms. Louise Massicotte, Assistant Director-General at the ADRLSSSM, has described the changes as a “rebalancing” from LTC facilities to other, less intensive solutions; 1,193 beds in intermediate-care facilities have been created and 500 more are planned before the end of 2012. All facilities must now be accredited and the inspection process is about 70% complete.
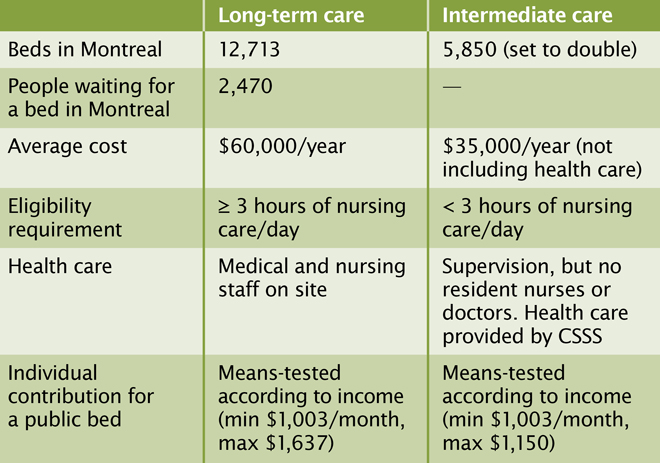
Source: Jacques Fournier, presented at a conference November 9, 2011, organized by the AQDR and partners in Montreal.
Many care providers in the community do not believe government has invested enough to ensure that people have access to appropriate care. Mr. Michel Clair, President of Sedna Health Group, describes an ever-increasing burden of illness among people admitted to LTC facilities, which has not been matched by additional funding per bed.
“Twenty years ago, when I was with the Association des centres d’accueil,” says Mr. Clair, they said that people could only be admitted if they needed fewer than two hours of care per day. Then it increased to two-and-a-half hours, then to three hours. Now, people coming into a CHSLD (LTC facility) often need four hours of care a day. In Ontario, budgets for nursing and nursing assistance in LTC take the heavier needs of the clientele into consideration using an automatic adjustment, but Québec still uses indexed historic budgeting.”
In evaluating the first stage of the project, the ADRLSSSM found that the number of people with specific needs, such as serious behavioural problems, was greater than anticipated and that there was a lack of spaces in the community for this group; that medical coverage was inadequate in a number of facilities; and that there was a perception that people were moved around more than before. On the positive side, there was an overall reduction in the number of days before a person obtained a place in a LTC facility.
Impact at the MUHC
The MUHC is meant to begin closing a number of beds on its transition-care units this year. Despite the transformations on the community side, in other hospitals where “PHPE” has been implemented to date, it has still not proven possible to place patients in an appropriate facility within 72 hours once the hospital informs the CSSS or ADRLSSSM that a patient is at the end of active care. The transition-care units at the MUHC were developed to provide an alternative to keeping patients awaiting placement in acute beds on other units.
Dr. Brown-Johnson has concerns that if or when these units close, delays in community placement could lead to historic levels of acute-bed blockages, which could compromise the MUHC’s capacity to meet its tertiary and quaternary care mandate. In order to mitigate this potentially paralytic impact, Dr. Brown-Johnson has spearheaded an initiative to develop an innovative hospitalist model of care at the MUHC, under the auspices of the Secondary Care Division of the Department of Family Medicine and in collaboration with the Department of Medicine, the OPHCCS, CSSSs and the ADRLSSS. The MUHC is exploring the possibility of keeping a small number of transition-care beds available, which would be incorporated into the proposed hospitalist care unit.
Dr. Brown-Johnson also describes a new problem that has arisen with the transformation. “Patients arrive in the ER from the new intermediate-care facilities,” she says, “often for behavioural disturbances. The geriatric consult team in the ER assesses the patient, makes some recommendations, adjusts the dosages of meds, etc., but often the facility refuses to take the patient back. A plan needs to be made to accommodate this group of patients.”
A number of hospitals have developed nursing and medical expertise in long-term and transition care. These positions are eliminated as patients move into community settings and these skilled and experienced practitioners are seldom successfully transferred to community LTC providers. At the same time, staff in community LTC facilities has to contend with more complex and more acute patients than before. The MUHC’s hospitalist model of care proposal includes the potential sharing of transitional care expertise with community LTC partners to help mitigate care gaps.
Redefining the hospital’s role
Even as their care for LTC patients diminishes, hospitals play important roles in easing transfers to community resources and ensuring that patients are in the best shape possible upon discharge. Dr. Nadine Larente has spearheaded the Elder-Aware Initiative at the MUHC Division of Geriatric Medicine to serve older patients well, not just in geriatric units but throughout the hospital. “An in-hospital approach that prevents at-risk older patients from deteriorating during their hospital stay can enable some to go home or require a lesser degree of care in a community LTC facility,” she says. The effort begins with identifying patients at risk (frail, confused, dehydrated, experiencing general deterioration, falling, etc.) right in the ER and aims to prevent or minimize delirium and functional decline in this group. Effective approaches look at all facets of the patient experience in the hospital and help these older patients with mobilization, orientation and eating.
Hospitals can also help improve transfers to alternate care by conducting detailed needs assessments that help the community resources determine where the patients should be transferred. Delays in placing people are often the result of community resources being unable to conduct timely needs assessments. “If we can provide that from the hospital,” says Larente, “the ADRLSSSM can respond much more quickly.”
Ms. Ann Lynch, Associate Director General, Clinical Operations and Nursing Affairs, MUHC, considers it essential that the MUHC continue to contribute to innovative ways of caring for patients who require an alternate level of care. “We will continue to work with our clinical partners in the community on the appropriate delivery of services for patients requiring long-term care in light of Ministry orientations,” she says. “Our tertiary and quaternary mandate requires that our system be able to respond to the population within our territory for these services, and additional efforts are needed to ensure that patients receive timely care in the right setting.”







