By Johanne Desrochers
This case study, prepared by the Health Innovation Forum with the collaboration of Johanne Desrochers, Associate Director of Telehealth at the MUHC, examines how the MUHC's Telehealth program served as the starting point for creating a virtual health and social services network. — Produced as part of the MUHC-ISAI's 2010 program.
Challenge
Providing specialized health services to people in remote regions is an ongoing challenge. The number of specialists and subspecialists is limited and the volume of practice outside major urban centres is insufficient to maintain skill levels. Academic health centres have traditionally provided consultation services to remote regions on a voluntary basis. In the province of Québec, this situation changed with the 2005 healthcare reform that created four integrated university healthcare networks (réseaux universitaires intégrés de santé or RUIS) and made each RUIS accountable by law for rendering specialized services accessible to everyone in its territory.
Johanne Desrochers, Associate Director of Telehealth at the MUHC, sees three ways to provide access to these services: “Either you move the patient to the professional in the urban centre,” she says “or you move the professional to the patient in the region, what we call outreach visits, or you provide services at a distance through telehealth.” Québec’s ministère de la Santé et des Services sociaux (MSSS) regarded telehealth as an important part of the new network structure and asked the four RUISs to come up with a master plan for telehealth development. “The healthcare reform changed the relationship we have with our partners in the North,” says Ms. Desrochers. “We always had a partnership based on goodwill, but now we have the legal obligation to find a way to meet their needs.”
The program
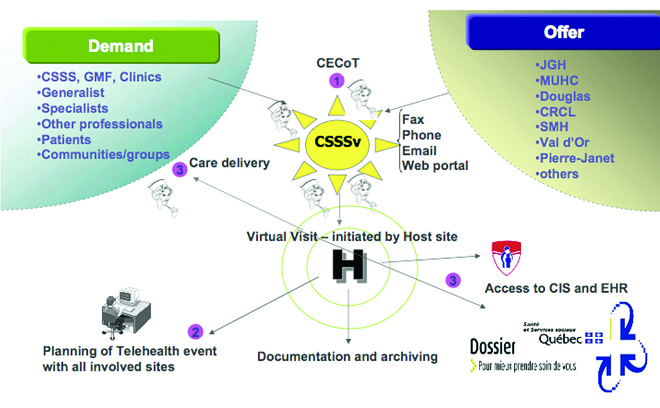
The vision Ms. Desrochers and her team were forging for the MUHC’s virtual health centre became the starting point for the model of a virtual health and social services network, the CvSSS (which stands for Centre virtuel de Santé et Services sociaux), that involved not just the MUHC but all partner institutions in the RUIS (see Figure 1). A RUIS McGill Telehealth Steering Group was founded and, in 2005, received Ministry funding to begin implementation of the CvSSS. The McGill RUIS Telehealth Network is defined as: “a network of organizations that provides or arranges to provide a coordinated continuum of clinical, educational and research telehealth services to a defined population, and is willing to be held clinically accountable for the outcomes of the population served.”
Telehealth is regarded as a strong driver in the network’s affairs, as it intensifies cooperation between network partners and improves coordination of resources and activities. The McGill RUIS Telehealth Network is governed by the McGill RUIS. The RUIS Centre of Expertise and Coordination of Telehealth (CECoT) is the operational arm of the CvSSS, acting as the single entry point of all requests for telehealth services, and supporting telehealth activities. A steering committee with representation from all the regions was set up to define needs and priorities. It identified four RUIS-wide priority areas for access to specialized telehealth services: cardiology, oncology, psychiatry and obstetrics.
Four RUIS clinical committees, made up of experts from the university-affiliated hospitals and the RUIS regions, were charged with defining the offer of specialized services within their field of expertise that will be made available through the CvSSS. Each committee must identify the subspecialties available among the RUIS experts in various health centres, and determine whether telehealth is an appropriate solution for the specialized services requested in the referrals. As well, the committees must try to estimate the volume of service requests expected to come from each region to support decisions about where to offer a given telehealth service. Finally, the committee must provide input into the balanced scorecard that will be used to evaluate the benefits of these new services.
The academic health centre’s subspecialty services must support and complement the specialized services already available in the regions. “Val D’Or may have an obstetrician,” Ms. Desrochers specifies, “but could turn to the academic health centre for subspecialty consults on high-risk pregnancies, for example.”
The clinical committee comes up with a final offer of services that is very concrete and looks essentially like a schedule for virtual clinics. Appointments are scheduled through the Coordination Centre (Figure 2), much in the same way that traditional referrals are made. Some of those clinics may be offered from regional hospitals. “If the hospital in Val d’Or wants to expand its offer of services in obstetrics, it will fall on the clinical committee for obstetrics to define what support is expected from the RUIS network to do that,” says Ms. Desrochers.
Once a committee has written the content of what will be available in the virtual health centre, Ms. Desrochers’ team is then responsible for organizing its delivery.
Clinical champions
Dr. Carolyn Freeman is Co-director of the Network’s Teleoncology Committee. Her interest in network solutions grew out of the problems in access to radiotherapy in 1999 that saw Québec patients being sent to the U.S. to receive timely treatment. “I got involved with the Ministry at that time to plan resource needs in radiotherapy,” says Dr. Freeman, “and that includes networking. It seems logical to me that we should be able to offer some services, and particularly education, by videoconferencing. So I was very enthusiastic when I was asked to get involved.”
In oncology, the RUIS involves three radiotherapy centres: the MUHC, the Jewish General Hospital and the Gatineau Hospital. They work together to provide services to patients throughout the territory. Telehealth expands collaboration in both direct patient care and education. “The MUHC runs weekly educational teleconferences attended by all doctors in the three centres ” says Dr. Freeman. Videoconferencing is also used for regular tumour boards, at which specific cases are examined by a multidisciplinary group. “These are especially valuable for very rare tumours, where expertise is concentrated in one or two urban centres,” adds Dr. Freeman.
In the provision of treatment, the academic health centres work with regional centres to enable patients to receive as much of their treatment as possible close to home. “They come to Montreal for their work-up and surgery, but then receive a component of their treatment elsewhere,” says Dr. Freeman. “We can assure the same quality of care because we continue to be linked with other clinicians and provide support.” She emphasizes that the point of the RUIS structure is not to centralize care but to treat the patient well as close to home as possible.
Referring doctors are asked to complete a ‘Web’-referral form, which is then forwarded to the Coordination Centre. The incentive for them to take on this task is that they receive a full electronic report from the consult within an hour of it being completed.
Uptake
The Coordination Centre has tracked a number of indicators to monitor the expansion of services provided by the MUHC Telehealth Network. Between 2004 and 2009:
• The number of participating sites grew from under 1,000 to 4,500.
• The number of videoconferencing sessions grew from 306 to 1,505.
• The number of clinical consults using videconferencing increased from 53 to 495.
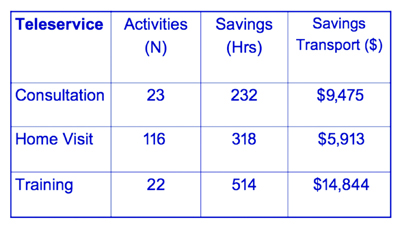
From 2008 to 2009, there was a 41% increase in real-time clinical consults and a 48% increase in educational sessions: 53% of all videoconferencing activity is in education. Figure 3 shows a preliminary view of the savings, in both dollars and hours, arising from telehealth activities.
Doctor participation
In the CvSSS, professionals provide their services as part of a network rather than a particular hospital. “That is a major paradigm shift,” Ms. Desrochers emphasizes. Doctors need to leave competition aside when they enter the telehealth world and move from an individual provider or hospital mentality to a network effort.
Creating the incentives for specialists to take on telehealth work is a challenge, especially as the Ministry does not currently allow most doctors to bill for such consultations. “The carrot,” Ms. Desrochers says, “is that the more we develop our services for virtual work, the more we can help the regions without having to move around patients or professionals.”
The willingness of urban specialists to adopt the new service delivery model often depends on whether they have had to spend weekends away covering for an understaffed service, or worked in these remote settings. “If so, they will be much more attentive to telehealth efforts,” ?Ms. Desrochers asserts. Not all specialists have felt the pressure. “When the MUHC hires new surgeons in Montreal,” says Ms. Desrochers, “they are told there is a possibility they may be asked to do outreach visits. It is not yet a matter of the department chief saying they have to go.”
Ms. Desrochers’ strategy is to forge ahead with the early enthusiasts. She recruited them onto clinical committees charged with defining the service offer in each of the four specialties identified by the regions. She appointed co-directors from different hospitals for the clinical committees to try and cultivate a new network culture.
Dr. Freeman also sees variation in the commitment of urban specialists. “People do not always know what their responsibilities really are in a service way. A lot (of departments) just keep their heads down,” Dr. Freeman finds. “They have very little interest in seeing what more they can do, because they are short staffed and cannot keep up with their current workload.”
Mixed remuneration models within an academic health centre make it easier for doctors to free up time for telehealth, as they can use the administrative or teaching time allotments for telehealth activities without losing money. The workflow needs to be as natural as possible. “It all has to be made easy for the patient and both treating teams,” says Dr. Freeman.
A systems approach
Ms. Desrochers emphasizes the need to look at the whole system: “What is the best way to set up your call system so patients can book an appointment? How do you make sure doctors have the clinical chart and the equipment they need on hand to conduct a particular examination? Does a nurse or doctor need to be present at the ‘patient’ end? A technician? How do we get the clinical report communicated back as quickly as possible to the treating physician? How will follow-up be arranged, by whom and with whom? We need a physical place on this end for the doctor, another for the patient at the other end, and communication between all the relevant personnel.”
The Telehealth Network recently received a budget from the Ministry to hire a clinical coordinator for each of the four specialty programs. The role of this clinician is to serve as the point person to receive the referrals, determine the urgency, ensure that the clinical information on hand is complete enough to set a date for consultation, and decide who should provide the consultation. “In oncology, we found a nurse with expertise in telehealth,” says Ms. Desrochers; “in obstetrics, we have a senior obstetrical nurse as coordinator.” They are just now beginning to define and develop these new network jobs.
Potential for expansion
Technical capacity
To fulfill its offer of service, the MUHC Coordination Centre needs to increase its capacity to respond to requests for consults, but also has to help increase local capacity in the regions. It therefore provides remote training to all telehealth users in the remote communities. But the manpower shortage is so significant that they are increasingly favouring systems that can be controlled from Montreal.
Financing
When Ms. Desrochers took on the telehealth mandate at the MUHC, she secured sponsorship for upgrading pediatric services from Operation Enfant Soleil. Bell came on board with a 10-year sponsorship beginning in 2007, to support building a virtual health centre that would serve the northern communities. Ms. Desrochers used the small operating budget provided by the MUHC to begin to offer services on the adult sites. A sustainable model for governance and financing telehealth across the RUIS was proposed by the Network to the Ministry in 2007 but has not yet come into force.
While the Ministry has just funded first costs of operating the Coordination Centre, it has not provided recurrent funding to the regions to expand their human resources dedicated to telehealth. “The regions are expected to find the funding from savings within their respective establishments — no new money,” says Ms. Desrochers. “However, the financial systems do not facilitate the recovery of the savings accomplished through telehealth — for example, savings from patient transport cannot be reinvested into telehealth.”
However, the infrastructure and processes that are being set up through the CvSSS to fulfill the requirements of the four priority programs will be the foundation upon which other telehealth programs will be run in the future.
Specialists
There is some concern at the Montreal regional board of health and social services (Agence de la santé et des services sociaux de Montréal) that wait lists will increase for Montrealers’ access to specialists if they devote more time to telehealth work.
Regional physicians
One ongoing challenge is to ensure that physicians in the regions are participating in telehealth program design and initiatives.
Dr. Freeman considers it of utmost importance to facilitate the introduction of new regional participants in specialized services: “In oncology, they need to be accommodated in terms of language and they need the technical capacity to present a case with pathology and imaging.”
The educational component is very important. The psychiatry group is offering a series of educational lectures, to be delivered via videoconferencing, to enable broad participation by regional providers. “We are now looking at that in oncology as well,” says Dr. Freeman.
Dr. Paul-Emile Barbeau, a general practice physician serving First Nations communities in Abitibi-Temiscamingue, describes telehealth consults as fantastic support to professional practice and continuing medical education: “I discuss with the specialist which protocol he decides on and why.” Consults also allow him to provide better and faster care to his patients.