By Andrew Wister
In this discussion paper, Andrew Wister, Chair of the Department of Gerontology at Simon Fraser University assesses the impact of aging boomers on Canadian health care. —Produced as part of the MUHC-ISAI's 2009 program
Baby boomers make up a considerable proportion of the Canadian population and the aging of the baby boomer cohort has captured the attention of health researchers, practitioners and policy makers. We know that health care intensity and costs typically escalate in the elder years. What, then, are the most likely scenarios in terms of population health and health care utilization as the boomer bulge moves up the age scale?
As we plan for the population’s future health care needs, we need to consider assumptions about the health characteristics of aging boomers very carefully. Will they be healthier than people the same age a generation ago? What will they need and expect from the health care system? These questions are key to determining courses of action that can equip our system for the future.
When will it hit?
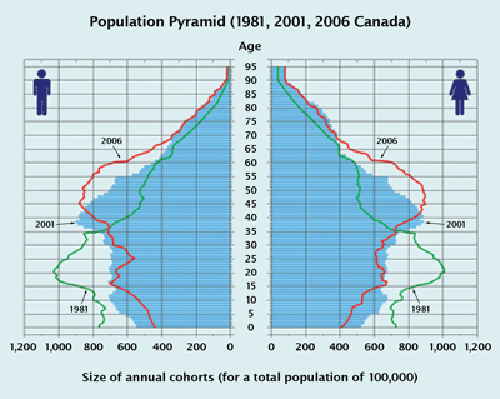
Boomers born between 1946 and 1965 make up approximately one-third of the population, or roughly 10 million Canadians. The front edge of this generation will reach their 65th birthday in 2011 (see Figure 1). By 2031, boomers will range in age from 65 to 85, with the largest bulge — those born between 1959 and 1961 — near the tail end of the boom. The largest boomer health care effect will not, therefore, be felt until this group reaches age 75 in the year 2035.
In 2006, 13.7 per cent of the population was 65 and over. This will rise to between 20 and 24 per cent by 2021. It should be noted, however, that the boomers are not a homogeneous group, varying by socio-economic status, life histories, and normative expectations. Some 17% of boomers are foreign-born.
Healthier seniors?
Some researchers believe that boomers will be healthier seniors than their generational predecessors because they are wealthier, eat better, exercise more, smoke less, and are more knowledgeable about healthy lifestyles. But this view is not universally accepted. A valuable place to start examining this assumption is by looking at health behaviours: they are malleable, and are associated with chronic illness prevalence and management, and ultimately with health care utilization. Reducing, delaying onset, and controlling chronic illness through preventable health behaviours at the population level may be our greatest opportunity to enhance population health.
Cohort analyses of national data sets in Canada between 1978/79 and 2004/5 indicate that, compared to persons their age in the previous generation, baby boomers have experienced a significant decline in smoking rates, inactivity and heavy drinking (more than 12/14 drinks per week for women/men). [1] However, obesity rates (BMI 30+) more than doubled from the previous to present generation. And while physical activity has improved over time among boomers, more than 50% are in the inactive category based on leisure-time activity measures. [2] Other health behaviours (i.e., exposure to stress, experimentation with illegal drugs, sleeping habits etc.) may also influence boomers as they age.
A review of studies examining eating habits suggests that the tendency for portion sizes to bulge and food quality to decline has likely cancelled moderate improvements in exercise level (and possibly some of the smoking improvements) for the boomer generation. The boomer lifestyle shows conflicting patterns, but the overall profile is likely better than that of earlier generations of seniors. However, there may be considerably more variability in morbidity and co-morbidity patterns among boomer seniors.
Chronic illness
Lifestyle can have an impact on some chronic illnesses and recent trends support this effect. The prevalence of chronic illness based on self-reports in national surveys indicates an increasingly complex illness landscape convoluted by age-related trends. If we compare the 1978/79 Community Health Survey (CHS) and the 1998/99 National Population Health Survey (NPHS), we see significant decreases in the prevalence of arthritis/rheumatism, hypertension, heart disease and bronchitis/emphysema in Canadians aged 45-64. [3] Among the same group, however, there were increases in the prevalence of diabetes, asthma, and migraine headaches.
Among people 65 and over, no decline in the prevalence of individual chronic illnesses was seen over that 20-year period, but rates of diabetes and asthma increased. [4] Comparing health care utilization data between 1985/87 and 1997/99 in Manitoba, Menec et al. [5] found that people 65 and over experienced fewer myocardial infarctions, strokes, cancer and hip fracture in recent years, but had higher rates of diabetes, hypertension, and dementia.
Dementia is among the greatest health care concerns of the future. The Canadian Study of Health and Aging estimates that approximately 8% of people aged 65 and over and about one-third of those aged 85 and over have dementia.6 Others project that dementia prevalence will reach 600,000 in Canada by 2021.
Compression of morbidity
The tendency for age-related disease to be compressed into a shorter period at the end of life, with a concurrent extension in life expectancy, is commonly referred to as compression of morbidity. The theory is that longer life expectancy doesn’t bring more years of disease, but rather pushes disease back farther towards the end of life. According to this scenario, longer life expectancy would be fairly cost neutral.
A large volume of research has looked at whether and to what extent there has in fact been a compression of morbidity. It may seem paradoxical that research shows a compression of disability among older people over time (using measures of functional disability, activities of daily living, or disability-adjusted life expectancy), alongside increased prevalence in some chronic conditions and functional impairments that require health care resources. The co-existence of these two trends can be explained by an improved health care system that diagnoses disease earlier, uses stricter diagnostic thresholds, and treats many illnesses more aggressively and effectively. It may also be attributed in part to better and more accessible community care and environmental designs that help extend independent living. Thus, older individuals are functioning better over time, despite reporting increases in certain chronic illnesses and more illness overall.
Coupled with these supply-side factors is evidence suggesting that people have increased expectations regarding health, health care services, and when they should relinquish independent living in the community.
The coexistence of these trends may be positive, but it is hardly cost-neutral.
Health service utilization
Over the last several decades, there have been apocalyptic forecasts regarding the impact of aging boomers on society. Ken Dychtwald, a well-known futurist in the U.S., contends that boomers are “a train wreck about to happen” due to a pandemic of chronic disease, mass dementia, in adequate pensions and pressures on a deteriorating health care system. [7]
In Canada, two patterns must be examined in order to address the likely impact of aging boomers on our health care system: 1) the effect of population aging on health care costs over time; and 2) changes in age-specific utilization rates.
In his article “Apocalypse No: Population Aging and the Future of Health Care Systems,” Bob Evans et al. (2001) analyzed administrative health care data from BC between 1975 and 1992 to try and answer these questions. [8] Evans et al. found that population aging accounted for only 10% of total health care cost increases over that period. Per capita expenditures rose by 26% in real dollars (about 1.4% per year), while the number of patient-days actually decreased for the total population of BC. Drivers of increased health care costs include a greater number of physicians per capita, a greater number of billings per physician, and a higher intensity of health service to the elderly, especially those over 75. This greater intensity has less to do with population aging, per se, than with increasingly expensive diagnostics and treatments. More sophisticated health technology produces improved health care, but also higher rates of illness.
A Manitoba study found that utilization rates have risen among older persons who are healthier — half of the reported increase in specialist consultations by older Manitobans from 1971-1983 was due to visits by persons in good health. [9] There is little doubt that an increasingly educated and health literate population results in greater use of a largely publicly funded health care system — the proportion of the population with post-secondary education has risen from about one-third to one-half over the last three decades.
Drug utilization
The increased use and cost of pharmaceuticals was found to be a significant driver of increased costs, with expenditures on drugs more than tripling between 1985 and 1999. Part of the increase comes from stronger doses and more complex drugs, but two therapeutic classes alone — hypertension drugs to control blood pressure and anti-lipidemic agents to control cholesterol levels — accounted for half of the increase. [10] These expenditures likely account for part of the paradoxical trend mentioned above whereby seniors live longer without disability, but still use proportionately more health resources for chronic conditions. The contribution of this spending category to overall cost increases makes it an important focus of attention, both to ensure that the drugs employed by “healthy” seniors offer good value, and that all Canadians have adequate access to proven ones.
Coverage for prescription drugs in Canada involves a mix of private and public insurance, and there is considerable variation between provincial drug plans. As drug costs escalate and pharmacare coverage decreases, some older people reduce or quit their medications because they can no longer afford them. Some seniors’ groups have advocated a national pharmacare plan but it has yet to receive sufficient support. The Romanow Commission on the Future of Health Care, [11] recommended a ‘catastrophic drug transfer’ plan to protect people who have excessively high drug costs owing to critical illness, but did not recommend national pharmacare. Rather, it proposed creating a National Drug Agency to evaluate and approve new prescription drugs, evaluate existing drugs, negotiate and contain drug prices, and provide comprehensive and accurate information about prescription drugs and drug usage to the public and to health care providers. Other approaches could involve wider implementation of the Beers List of appropriate and inappropriate drugs for the elderly.
In preparing for an aging boomer population, Canadian governments will need to pay much greater attention to pharmaceutical policy. There is a need to examine ways to reduce the amount of unnecessary or ineffective prescriptions, without compromising the benefits that appropriate use of drugs brings to the health of Canadians.
Hospital stays
There would also appear to be a significant overuse of hospital stays for elder Canadians. De Coster et al. [12] studied costs related to inefficiencies in current health system organization in Manitoba and found that 42% of days spent in hospital among persons aged 75 and over were spent either awaiting transfer to another level of care (a nursing home, for example), or waiting for medical tests or treatments. This study also found that 40% of hospital days in the province were used by 5% of long-term stay patients, of whom two thirds were 75 and over.
Shaping the future
There has been a relatively slow increase in population aging over the last few decades, but it will rise significantly as the baby boom generation becomes elderly. Although it has been established that population aging has not been the driving force behind escalating health care costs over recent decades, we would be remiss to underestimate the impact of the coming bulge in our senior population.
We can expect more users of health care in the coming years. The front end of the baby boomers will reach age 75 (a key marker of health care utilization) by 2021, and by 2035 the entire boomer generation will be in the age range of high utilization.
What to expect in terms of age-specific utilization patterns is less clear. While some risk factors (especially smoking) are much less prevalent, high obesity rates will likely continue for some time. Increasing rates of diabetes, asthma, dementia and certain cancers may cancel out savings from lower rates of other diseases.
The observable compression of disability should not be equated with lower health care utilization. Modern medicine has succeeded in weakening the link between morbidity and disability. Furthermore, it is likely that individual care expectations, coupled with rigorous treatment protocols by medical professionals, will fuel a highly medicalized health care system characterized by increasing medical testing, prescription use and advanced treatments.
These trends suggest the need for a more flexible healthcare system that can respond to significant shifts in population health as the boomers age over the coming decades. While the boomer generation may be demanding, it is also adaptable, technologically savvy and open to innovation. Senior boomers will be more amenable to new health technologies, such as telemedicine, e-health or Internet-based prevention or monitoring systems that may keep them healthier. [13]
Boomer spending on anti-aging products and programs is significant and may indicate greater willingness to pay out-of-pocket for greater utilization of a greater variety of health care services and treatments. This may exert pressure to shift from the current 70/30 per cent public/private funding formula to one that allows for greater private spending on care that goes beyond what the public system can reasonably afford.
The key will be to balance the integrity of the health care system inherent in the fundamental principles of the Canada Health Act with the need to find health care efficiencies and control costs. Innovations and changes to the current system need to be thought through, implemented and evaluated very carefully.
We are not the only country experiencing population aging and health care pressures. Many Northern European countries have gone through this process ahead of us. In the UK, significant changes have been made in a short period, with the adoption of a salaried system for physicians, and use of financial incentives to encourage them to lower patients’ risk factors. It appears that financial motivators are effective levers to shape health care delivery as well as individual demand.
As we look into the future and attempt to forge a long-term vision for our own health care system, changes are needed to address the very complex patterns of illness and expectation that underlie boomers’ future health care utilization.
Priority areas for government
- increase population health efforts, especially those targeting eating habits, obesity, and physical activity levels
- develop dementia treatment and care efforts
- find cost-effective ways to prevent and manage chronic conditions
- better understand health utilization among ‘healthy aged’
- improve evaluation and coverage of prescription drugs
- use new technologies, such as telehealth and electronic medical records for tracking and research
- examine the private-public funding mix of the health care system
_____________________
Dementia care
It is not clear whether the growing numbers of Canadians with dementia reflect increasing incidence of the disease, a greater number of older people or a high proportion of false positives in testing for early-onset dementia. Regardless, our health care system must prepare for rising demands on dementia care, and develop more innovative and effective ways to prevent and treat the disease. A number of integrated health care delivery models have provided health care, housing and social services to frail elderly patients through better co-ordination between the acute, continuing, and long-term care sectors. Demonstration projects in Quebec have shown that these integrated services cost significantly less than usual care, as they enable some patients to be directed from hospital and institutional care to less expensive community care. [14] Integrated models typically share a number of features:
- single entry point
- case management
- geriatric assessment by a multi-disciplinary team
- co-ordination of hospital, nursing home care, and home care
- standardized assessment instruments
- simplified payment system
___________________________
References
- Wister, A.V. 2005. ‘Baby Boomer Health Dynamics: How Are We Aging?’. Toronto: University of Toronto Press.
- 2006. Leisure-time Physical Activity, by Age Group and Sex, Household Population Aged 12 and Over Canada, 2003. Retrieved February 14, 2006 from http://www.statcan.ca/english/freepub/ 82-221-XIE/tables/html
- Statistics Canada. 1999a. ‘Health Among Older Adults’, Health Reports, 11(3),47-6, Cat. #82-003.
- 1999b. ‘Health in Mid-Life’, Health Reports, 11(3), 35-46, Cat. #82-003.
- Menec, V. et al., 2005. ‘Trends in the Health Status of Older Manito-bans, 1985-1999’, Canadian Jour-nal on Aging, 24(Suppl.1), 5-14.
- Hogan, D. et al. 1999. ‘Disease, Disability and Age in Cognitively Intact Seniors: Results from the Canadian Study of Health and Aging’. Journal of Gerontology: Medical Sciences, 54A(2), M77-82.
- Dychtwald, K. 1997. ‘Wake-up call: The 10 physical, social, spiritual, economic and political crises the boomers will face as they age in the 21st century’, Crit-ical Issues in Aging, 1, 11-13.
- Evans, R., et al. 2001. ‘Apocalypse No: Population Aging and the Future of Health Care Systems’, Canadian Journal on Aging, 20 (Supp. 1), 160-91.
- Black, C. et al. 1995. Rising use of physician services by the elderly: The contribution of morbidity. Canadian Journal of Aging 14(2), 225-244.
- Grootendorst, P. et al., 2003. ‘A Review of the Comprehensiveness of Provincial Drug Coverage for Canadian Seniors’, Canadian Journal on Aging, 22(1), 33-44.
- Romanow Commission. 2002. Commission on the Future of Health Care in Canada.
- De Coster, C. et al. 2005. ‘Use of Acute Care Hospitals by Long-Stay Patients: Who, How Much, and Why?’, Canadian Journal on Aging, 24 (Suppl.), 97-106.
- Sinden, D. & Wister, A.V. 2008. ‘E-health promotion for aging baby boomers in North America’. Gerontechnology, 7(3), 271-278.
- Béland, F. et al. 2006. ‘Inte?grated Services for Frail Elders (SIPA): A Trial of a Model for Canada.’ Canadian Journal on Aging 25(1), 24-42.