By Antonia Maioni
Antonia Maioni assesses the net effect of federal and provincial healthcare reports over the last decade. —Produced as part of the MUHC-ISAI's 2008 program
In the past decade, every Canadian province has published at least one health care report. Some, like the Clair Commission report in Québec (2001), have been very broad and elaborate. Others, such as the Ontario Hospital Restructuring Commission (2000), were more specifically targeted. The more controversial reports, such as Don Mazankowski’s for Premier Ralph Klein in Alberta (2002), have resonated long and loud in health reform circles.
During the same period, the federal government (under Jean Chrétien’s Liberals) commissioned two major reports. The National Forum on Health (1997) was designed to find out what was right about health care in Canada. The Commission on the Future of Health Care in Canada (2002), chaired by Roy Romanow, sought to identify challenges and remedies. In the context of framing health care reform as a cost crisis issue, even the Senate of Canada flexed its political muscle by mandating the Standing Committee on Social Affairs, chaired by former Senator Michael Kirby, to survey and report on health as well (2002).
Major-league commissions, extensive research budgets, thick and voluminous reports, dozens upon dozens of recommendations… to what end?
Have commissions changed health care?
The debate over health care reform has shifted substantially in Canada over the decade, though whether this is a result of commission activity or a reason for it is difficult to ascertain. The key recommendations from each of the major commissions, along with key actions taken by various governments over the decade are presented in a separate article.
On the one hand, the debate has become much more infused with evidence. One of the major contributions of the Romanow commission was the 40-odd research papers published alongside the report. We know more than ever before about the social determinants of health, the impact of evidence-based medicine, the structure of public opinion, and the real access issues affecting Canadians. On the other hand, the debate has polarized substantially, leading to often unhelpful dichotomies between “public” and “private,” between less and more spending, between federal and provincial roles and responsibilities.
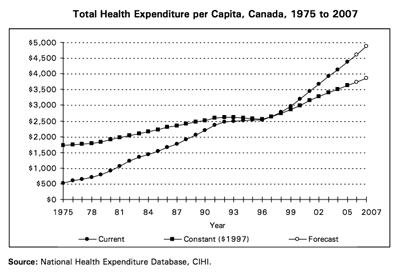
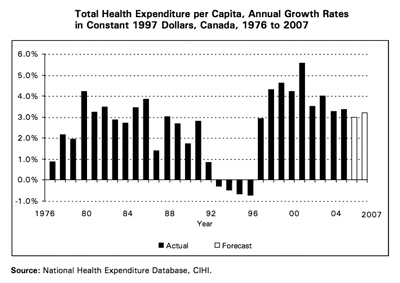
Political leaders used to consider health care the crown jewel in the Canadian welfare state. But as one commission after another pored deeply — often with an abrasive approach – into the health care system, some of that shine rubbed off. The major shocks administered to health care during the period of austerity in the mid-to-late 1990s (see Figures 1 and 2) sullied the playing field even as it came under intensive scrutiny. Health care budgets were slashed and providers and patients were forced to adjust without a plan.
Public opinion polls tell us that confidence in the system has eroded over the decade and there is increased anxiety about the sustainability of public funding. There has also been an erosion in people’s confidence in policy-makers, partly due to the steady drum-beat of reform-speak that persists without producing a clear consensus on the direction of change. Given that environment, it has been difficult to act on many of the recommendations put forth by commissions and much about health care has stayed the same.
Nevertheless, specific legislation has emerged in most provinces emanating from these commissions and reports, and the federal government has also taken some heed. It can also be argued that the Senator Kirby’s report influenced the Supreme Court in its landmark Chaoulli ruling on private health insurance.
In Québec, the Clair commission prompted an overhaul of regional boards, sounded the alarm about an aging population, and jump-started primary care reform (although the project is still very much in progress). Pilot projects for vulnerable elderly were instituted but did not survive.
In Ontario, substantial change in the hospital sector, including regionalization, followed the Hospital Restructuring Commission report, but it is difficult to say that this was a direct consequence of the report.
In Alberta, the Mazankowski report succeeded in changing the debate but not necessarily legislation. Bill 11, which expanded possibilities for private health care delivery, preceded the report but likely gained legitimacy following its publication.
Federally, the National Forum on Health emphasized health and medical research and prompted the creation of the Canadian Institutes for Health Research (CIHR) (replacing the Medical Research Council and other research funding groups) and the Canadian Institutes for Health Information (CIHI). It was the first to raise the importance of developing electronic health records, a goal that has not yet been achieved.
The Commission on the Future of Health Care in Canada recommended and was successful in seeing implemented a significant federal reinvestment in health spending. Multiyear funding was set at a level higher than recommended; a federal-provincial accord was signed, and specific health funds established in targeted areas such as wait time reduction and primary care. As per recommendations, a Health Council was established but its use and clout remain uncertain.
Provinces have responded to calls for a renovation of primary care, though home care and a national Pharmacare programme, which were both subject to recommendations in the report, still lack political traction.
What’s different about the latest wave of reports?
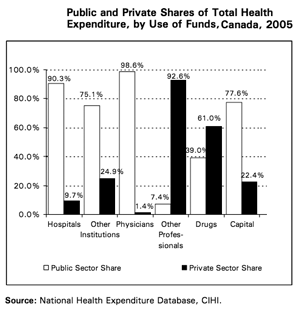
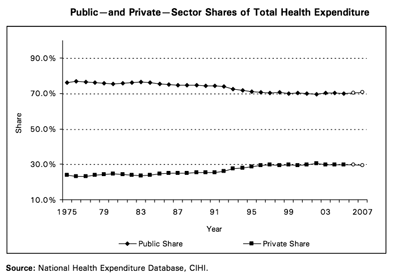
The latest wave of health commission reports differs in that these raise the possibility of – and in some respects, the preference for – an array of private-sector initiatives or public-private partnerships as solutions to the challenges of health reform. Figures 3 and 4 present the trends in and breakdown of private spending. For example, the Ménard report in Québec (2005) suggested drastic financial measures to respond to what was an apocalyptic projection of future health costs. The more recent Castonguay report (2008), meanwhile, recommended creating the conditions for a parallel private market by providing the insurance industry a larger role to cover a broad range of services and allowing physicians to practice both in the public system and the private market.
To some extent, these controversial reports are more a reflection of the current tenor of public debate and partisan politics than a motor of change per se. Their recommendations on financial matters are unlikely to see the light of day in the short term. For now, the Québec government has limited itself to allowing private insurance for cataract, hip and knee surgery, and did so only to comply with the Supreme Court decision in Chaoulli vs. Québec, not in response to specific commission recommendations.
There is still no consensus on the accuracy of the analysis regarding our current situation (particularly the doomsday scenarios of aging and the funding crisis) presented in the Québec reports. Interest group opposition (largely resulting from the way in which unions and professionals have invested in the public system) make it difficult to move in the direction proposed in these reports. The virulent reaction to the Castonguay report also raises the spectre of tax-payer revolt. It is one thing to ask someone in an opinion poll whether they support user fees, another thing to actually “price” the individual deductibles or sales tax increases as Castonguay did.
One of the substantive impacts of the Chaoulli ruling has been to emphasize the problems inherent in the use and misuse of evidence and comparative analysis. This is a common theme in social science literature and is well-illustrated by discussions in Kirby, Castonguay and the BC examples. In the Supreme Court deliberations on Chaoulli, it was the absence of concrete evidence about the relationship between waiting lists and private insurance in Québec that led the Court to look for guidance in the Kirby and Romanow reports. And those reports’ different interpretations of the evidence led to the Court’s divided judgment on the untested notion that limiting access to private insurance is a legitimate means of protecting collective access to public health care.
Following the Court’s decision, the idea that private insurance poses no threat to public health was taken up in the Castonguay and BC commissions this year, leaning on one possible interpretation of comparative analyses of other industrialized health care systems – specifically, that such examples provide evidence that privatization and universality can co-exist. Again, there is no consensus that this is in fact the case, or indeed that the co-existence of private markets for health care has contributed to cost control in the comparator countries.