By Claude E. Forget
Claude E. Forget, a pioneer in the design, implementation and study of health and social services in Québec, traces the evolution of government’s role in health care to see where our system is heading today. —Report from a presentation at the 2008 conference of the MUHC-ISAI
My purpose here is to provide some perspective on what governments have done in the past, and from there extrapolate what they are likely to do next. Policymaking is often portrayed as reflective of the unpredictable and opportunistic nature of partisan power struggles but more meaningful patterns are observable on a longer-term basis.
Inescapable realities and widespread perceptions shape policy. Changes in circumstance will force changes in policy, even when these only take effect after lengthy delays. Government may have limited scope for imaginative policymaking, but it can and should exercise leadership by shaping public perception of change.
Government’s core functions
Governments have many other concerns besides health care, some of which have a prior claim on public resources: national infrastructure, the justice system, education and poverty relief programmes all come to mind. Each supports the operation of the economy while working to ensure the protection of the rights of individuals. The ability to effectively manage concerns like these is the criteria that distinguishes a successful state from a failed state. It also contributes to the health of the people: the incidence of many diseases fell markedly thanks to economic and social development even before the advent of modern medicine.
Turning more specifically to health, we see demand for public health programs steadily increasing. Policies on pollution, toxins and communicable pathogens, workplace, and consumer health and safety measures — everything from compulsory seat belt laws to anti-smoking measures to the regulation of prescription drugs — and the enforcement of these policies represent the core of government’s role in health promotion. This is a field where only state organizations can be effective: health care with the entire population as the patient.
The state contributes significantly to the health of the population as it pursues mandates that, by their very nature, are exclusive to the state. Governments are compelled to give priority to those tasks which are key to their raison d’être, largely because they are the only agencies through which these core tasks can be performed. Personal health care does not belong to this core, though governments can choose to become involved, as they have in Canada and most European countries. However, when this involvement conflicts, at least financially, with government’s core functions, partial disengagement will take place. It may be gradual and covert, but it is inescapable.
A little history
In Canada, the history of provincial government involvement in health care services goes back to the 1920s. When, in the late 1950s, the federal government decided to jump in, it was not through any desire to assume responsibility for health care delivery (an intention explicitly denied at the time), but to shield families from the financial repercussions of serious illness. The same was true about the introduction of Medicare a decade later. Legislation first referred to “hospital insurance” and then to “medical and diagnostic services insurance,” clearly defining the limited ambition at the origin of those programs, namely to pay for services rendered and controlled by third parties.
This is where matters stood until the early 1980s, when Parliament passed the Canada Health Act (CHA). Over the 25 years since, the concepts of universality, comprehensiveness, public administration and portability spelled out by the CHA have taken on a different meaning than they had originally. Designed as administrative protocols, comprehensible only in the context of cost-sharing arrangements between the federal government and the provinces, they have now become the “principles” guiding the Canadian health care system — the word insurance having disappeared from the official vocabulary along the way. The effect has been to create a whole new set of expectations on the part of both bureaucracies and the public, centred around the notion of a governmental guarantee of individual rights to health care. It is no accident that the CHA became law just a few years after the federal government altered the basis of its financial responsibility for health care from cost-sharing to flat per capita grants determined arbitrarily through “negotiations.” In essence, the CHA saw the federal government make a commitment on behalf of the provinces, albeit without asking them. For the feds, it was politically a very attractive trade-off.
The provinces, from that point on sole “equity owners” in the system, became increasingly involved in managing health care. All kinds of restructuring initiatives were taken, such as regionalization, community clinics and so on, but empirical evidence remains sparse as to the effectiveness of the many changes carried out. More importantly, after nearly 30 years of overt attempts to manage provincial systems, they are still not stable or sustainable. This worrisome outcome results from the convergence of three probably uncontrollable and partially self-imposed factors I like to call the “Bermuda Triangle” of health care.
The Bermuda Triangle of health care services
Scientific advances
On the first side of this triangle are scientific and technological advances that can be applied in health care. In the US, for example, $100 billion has been spent annually on medical research and development (R&D) since 2005, with the world as a whole spending close to double that amount. From this gigantic effort have come the drugs, devices and knowledge responsible for revolutionizing medical care. News of discoveries and innovations quickly disseminates internationally in today’s hyper-connected world, pushing standards of care ever higher.
Studies disagree about the impact this steady flow of innovation has on health care costs. Some attribute 70% of cost increases over and above inflation to innovation; others believe it is more. What is certain is that scientific progress is not cost-neutral, given that innovations are invariably about doing “more” and doing it “better.” Even innovations such as non-invasive surgery or better anaesthesia, which were originally believed to offer a cost reduction by shortening hospitalization, have been shown to increase overall costs because they expand the pool of surgical patients to include those who would have been too frail to undergo more invasive procedures.
Today, we stand on the cusp of much more radical medical change. What genomic research tantalizingly offers for the future are cures that currently seem miraculous: designer drugs, the regeneration of severed limbs and the repair of central nervous system cells. Personalized medicine, as this is sometimes called, may or may not live up to expectations, but some of these miracles may be achievable within the coming decade. This will not be cheap.
Consumer culture
The second side of the “Bermuda Triangle” reflects the gradual rise in standards of care, a phenomena quite distinct from R&D. The dictum, “Do no harm” has always been one of the cornerstones of medical practice, but over the past few decades the health care community has taken concerted action against medical errors. Care is rationalized through evidence-based analysis, multidisciplinary collaboration and patient consultation, and the emphasis is placed on the quality of care. The drive to raise standards in health care reflects our culture’s consumer orientation. We live in a world of ombudspersons, consumer protection agencies and class action law suits. In our globalized world, what is available elsewhere must also be made available here.
This increased consumer orientation in health care is apparent in the changing treatment of the CHA. In the early 1980s, the CHA was considered to spell out a number of “principles.” Politicians of all stripes have since treated these principles as the Holy Grail; recently, they discovered the principles are legally enforceable. The Chaoulli v Québec decision of 2005 ruled that a patient should not be made to wait unnecessarily for care. Today, governments are compelled to take steps to prevent unnecessarily long wait times and to provide diagnostic and therapeutic procedures that are in common usage in other rich countries.
Higher standards of care in terms of safety, timeliness and responsiveness act synergistically with new technologies to increase costs.
Inherently stagnant productivity
The third and final side of my “Bermuda Triangle” represents the inherent tendency of health care (even with static technology and stable standards) to see its costs rise relative to other sectors of the economy. This is because health care is strictly a service industry. In sectors such as mining, agriculture and manufacturing, volumes of production have risen despite the steadily decreasing share of the labour force they employ. In other words, productivity has increased. Although the human resources of the health system have not decreased relative to what they “produce,” the incomes of health care personnel have nonetheless tended to rise alongside pay rates in other sectors that have seen productivity gains. The end result is that health systems cost more and more relative to the rest of the economy. Neither do we really want the productivity of human resources directly involved in care to increase as this would reduce human contacts between caregiver and patient.
Hurricane watch
The factors that make up health care’s Bermuda Triangle are good things in and of themselves. We welcome the flow of ideas, techniques, equipment and medicines that make effective new treatments possible. We participate in the global research effort, applaud patient-centred care, and enable our courts to ensure that large-scale government programs follow guidelines and principles. It is also essential that remuneration and working conditions in a sector as important as health care remain commensurate with other parts of the economy in spite of the absence of “productivity gains.” However, with the growing importance of all these good things, the slow vortex at the centre of the Bermuda Triangle risks becoming a hurricane. With so many blessings, will we be able to sustain our present system?
Single payer restraint
The superiority of the Canadian “single payer” system for financing health services has often been extolled, particularly in comparison to the American situation.
A generation ago, when I was Québec’s Minister of Health, I used the term “rationing” at a press conference. What I said was that with the arrival of Medicare and the removal of price mechanisms regulating access to services (even after hospital insurance was introduced, a fee had been charged for ambulatory visits), another rationing device had to be put in place. To the naïve former professor of economics that I was, rationing was literally a mechanism to ensure equitable universal access to scarce resources. The following day’s editorials were scathing!
Despite this country’s distaste for the notion, rationing is common practice. Some methods are clear enough: hospital closures, budget cuts, funding delays, restrictions on available drugs, and ceilings on medical school enrolments and residency positions are all forms of rationing. While never openly acknowledged as rationing tools, such practices have contributed to controlling costs to a certain extent. Government cost control practices contrast very sharply with the brutal techniques used by private insurers in the US.
But these methods to restrain the escalation of government’s financial contribution have not been sufficient in themselves. There is evidence that other mechanisms are also at play.
Conservative use of resources
OECD data report that for procedures such as heart bypasses and dialysis, the rate per 100,000 people is twice to three times higher in the US than in Canada. Could this reflect that health care professionals here have a more conservative approach to the use of diagnostic and therapeutic procedures?
Optional private services
However closeted, there has also been growing recourse to a two-tiered approach, to the point that this reality has won quiet but fairly widespread acceptance. The action takes place largely outside hospital settings where wait times for certain procedures can be drastically and legally shortened using out-of-pocket payments. However, hospitals also offer a galaxy of “optional” embellishments over and above what governments pay for, including certain prostheses in ophthalmology and orthopaedics, contrast media in tests, and various drugs. The legitimacy of optional offerings remains a matter of continual interpretation.
Private donations
Private donations continue to play a vital role, as they did before Medicare, especially in that area most clearly underfunded by governments, namely the infrastructure of our institutions and their growing capital intensity as they require ever more elaborate equipment.
Private delivery
Policy response to the Chaoulli v Québec decision has brought increased public financial commitments to shorten wait times for specific procedures by using and paying for extra services in private clinics. This response, meant to preserve the integrity of the public system, demonstrates how difficult it is for that system to adapt even when given an express mandate to do so.
Medical tourism
Medical tourism is emerging as a potentially pivotal factor in reducing public sector costs. This year in the US, about one million Americans will go abroad to receive treatment at a fraction of US costs. Private insurers support this. Could hard-pressed Canadian governments ever do so as well?
Intensity of utilization
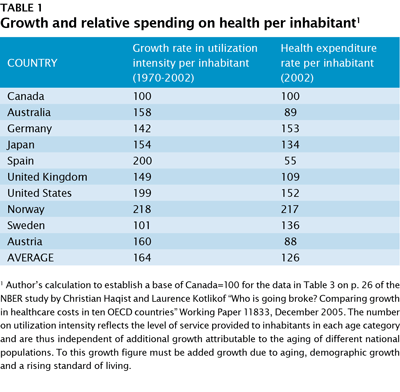
It does appear that Canada has been more successful than most other countries at controlling its health care costs. A study by the National Bureau for Economic Research, published in 2005 and based on Organization for Economic Cooperation and Development (OECD) data, surveyed health costs for 10 countries over the period 1970 to 2002 (Table 1). In Canada, the increase in the intensity of utilization of health care services has been below the average increase of all comparator countries. As a result, the level of health care expenditures in Canada in 2002 was 25 percent below the 10 country average, and well below the level of per capita expenditure in countries such as Sweden, Norway, Germany, the US and Japan. The phrase, “increase in the intensity of utilization,” refers to the increase in expenditure after deducting the impact of aging, population increase, and economic growth. It is a “pure” increase in utilization in a hypothetical world where nothing else changes.
These figures relate to total expenditures financed from either public or private sources. They indicate that private expenditures contribute to higher overall spending and fail to moderate any increase in public expenditure: public expenditures for health increased more rapidly in most other countries than they did in Canada over the same time period.
The figures show what happened rather than what should have happened. Is the lower level of Canadian expenditure optimal or does it reflect a need for a catch-up phase?
The squeeze is on
Even with its relatively low growth rate for total as well as publicly-financed health care, the Canadian rate of increase in spending is still higher than our economy’s growth rate by a margin of two to three percentage points. This implies that public expenditures for health gradually squeeze out other public spending responsibilities, many of which sit closer to the core of government’s essential role.
The obvious response would be for government to increase taxation and make the public system work more efficiently. Health care has, after all, been identified repeatedly as a top priority by the Canadian public.
However, government has not raised taxes, and appears unlikely to do so in the near future. In the 1980s, when the increase in health care costs was particularly rapid, governments allowed deficits to balloon rather than raise taxes, and when the deficit became impossible to sustain, it was health budgets that were reduced, not taxation that was increased. Today, there are new and cogent reasons to believe that an increase in taxes to finance the public system of personal health care is even less likely. With China and India finally within reach of standards of living remotely comparable to our own, the era of cheap and abundant food and energy has disappeared, perhaps forever. At the same time, wages in those countries are increasing rapidly along with their exchange rates so that the era a cheap manufactured goods is also on the wane. The pressures on our own standards of living are therefore multiple and long-term. This is not a political environment propitious to increased taxes. Other means of relieving the pressure must be found.
What comes next?
How is government’s role in health care likely to change, given these factors? The first order of business is to stop lying to ourselves. We have a major problem on our hands; namely, how do we sustain unchanged the totality of a system that, taken to the letter of the law, promises virtually everything to everybody?
Barring a miracle in the development of knowledge, I believe this state of affairs will inevitably result in the public system of personal health services reducing the services it covers by a sizeable margin. Not 10 or 15 per cent, but as much as 40 percent.
If we are to accomplish this inevitable retraction of a public system that promises all services (the “comprehensiveness” principle) to everyone (the “universality” principle), a choice will need to be made. I think and hope that universality will be maintained and comprehensiveness sacrificed. However, I may be unduly influenced by my own preferences rather than probabilities in saying this.
Whatever happens will be shaped by our healthcare system’s peculiar structure of governance. To call it a single payer system is a misnomer; in effect, it is a dual-payer system. It cannot undergo major modifications without the provinces and the federal government reaching agreement on a difficult and politically explosive issue. Any conceivable scenario will be made more problematic by the disparate incentives to which federal and provincial politicians respond. Provincial politicians are motivated by a single imperative: avoiding the breakdown of the “legacy” system they run, which would be a catastrophe for the citizens but a source of acute embarrassment and potential defeat for themselves. Federal politicians are motivated by the desire to appear helpful while taking care to shoulder as little as possible of the risks and costs of that legacy system. This leads them to favour marginal and time-limited financial commitments for narrowly defined and “innovative” purposes.
In times of change, rigidity in policy-making is the worst of curses. Life moves on; those who cannot anticipate required changes and proactively adapt are ultimately destined to disappoint. The broken governance structure for the Canadian public system for personal health care should be seen as the first issue to address. This is not happening.
Forecasters always take the long view. Predict the weather, promise rain or sunshine, and you are bound to be proven right just so long as you do not say when. I shall therefore make no prediction about what will happen to the government’s role in financing personal health care services, but I will venture to says that within the next five to seven years major changes will take place. Stay tuned.